Interstitial Lung Disease
Author(s): Osman El-Koubani
Learning outcomes:
- Revise the histology of lung parenchyma
- Describe the clinical features of interstitial lung disease
- Categorise the interstitial lung disease into subgroups
- Review the causes and histological features of granulomatous lung disease
- Describe the clinical and histological features of hypersensitivity pneumonitis
- Recognise the known causes of interstitial lung disease, particularly asbestos exposure
- Describe the classical features of idiopathic pulmonary fibrosis
- Describe the classical features of other common types of idiopathic interstitial pneumonitis
Lung Histology Part 1 of 14
Lung parenchyma is the areas of the lungs involved in gas transfer including the alveoli, interstitium, blood vessels, bronchi and bronchioles. Damage to any part of the lung parenchyma can lead to interstitial lung disease.
Lung interstitium comprises of alveolar epithelium, pulmonary capillary endothelium, basement membrane, perivascular and perilymphatic tissues.
Recap of the path air takes when inhaled:
- Respiratory bronchioles: final division bronchioles within the lung from which alveoli branch off, therefore this is where gas exchange can begin
- Alveoli: where gas exchange occurs – it has a scaffolding of collagen and elastic fibres that allow it to expand on inspiration
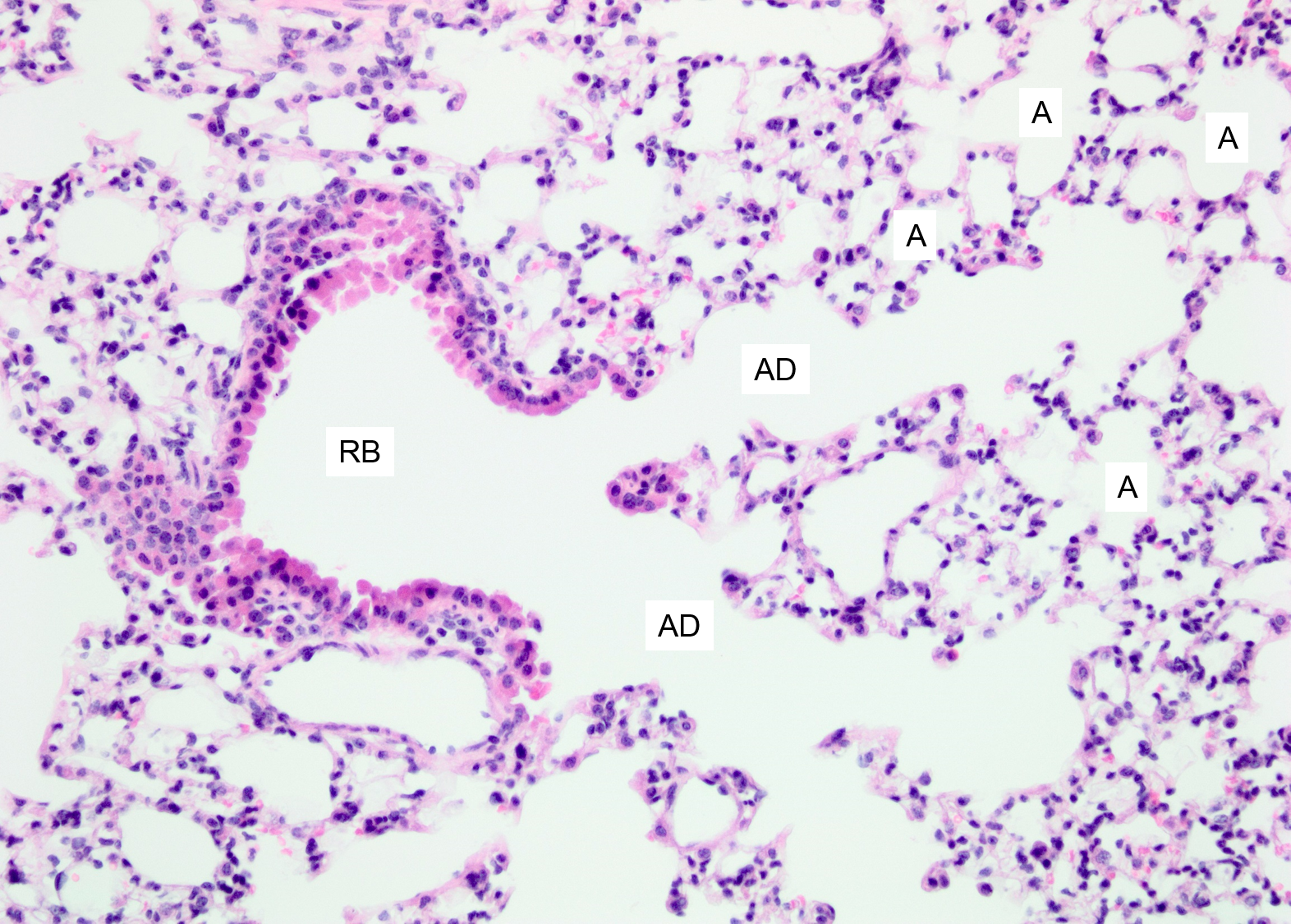
RB = respiratory bronchiole
A = alveoli
AD = alveolar ducts
Clinical Features Part 2 of 14
A patient may present with:
- Shortness of breath
- Cough
- End-inspiratory crackles
- Finger clubbing
- Cyanosis
- Pulmonary hypertension leading to cor pulmonale (right-sided heart failure)
Investigations:
Pulmonary function tests/spirometry: Show restrictive pattern
| Forced vital capacity (FVC) | ↓ |
| FEV1*/FVC |
Normal / ↑ |
| Transfer factor | ↓ |
*FEV1 = forced expiratory volume in 1 second
Chest X-ray:
Chest CT:
Subgrouping Part 3 of 14
Interstitial lung disease can be divided as follows:

Alternative Subgrouping by Location Part 4 of 14
Another useful way of clinically subdividing them is by location:
Signpost Part 5 of 14
We will now look at these groups, in turn, starting with known causes

Granulomatous Causes Part 6 of 14
Granuloma = collection of histiocytes and macrophages +/- multi-nucleated giant cells.
These can be split into caseating or non-caseating granulomas.
Caseating causes
- Infective: (more common in immunosuppressed patients)
- Bacterial – TB, Pneumocystis jiroveci
- Fungal – Aspergillus, Histoplasma, Cryptococcus
Non-caseating causes
Necrotising:
- Vasculitis:
- C-ANCA / anti-pr3 positive = Churg-Strauss syndrome
- P-ANCA / anti-MPO positive
- Nasal involvement = Wegener’s granulomatosis
- No nasal involvement = microscopic polyangiitis
Non-necrotising:
- Sarcoidosis
- Hypersensitivity pneumonitis*
Hypersensitivity Pneumonitis Overview Part 7 of 14
Hypersensitivity pneumonitis is a type III hypersensitivity reaction. Therefore Antibody/Antigen complexes form within the lungs → widespread alveolar inflammation (alveolitis).
Various causative agents:
- Farmer’s lung
- Pigeon fancier’s lung
- Mushroom picker’s lung
- ‘Hot tub’ lung
Clinical features:
Acute
- Systemic symptoms e.g. fevers, shortness of breath, cough, chest pain
Chronic
- Persistent productive cough
- Finger clubbing
- Weight loss
Hypersensitivity Pneumonitis Histology Part 8 of 14
Prognosis:
Most resolve when exposure to the agent is removed but can be chronic and lead to established fibrosis.
Non-Granulomatous Causes Part 9 of 14
Non-granulomatous known causes of interstitial lung disease include:
Known non-granulomatous causes
Known non-granulomatous causes of interstitial lung disease include:| Inhaled irritants/pneumoconiosis | Systemic disease | Iatrogenic |
|---|---|---|
| Asbestosis* | Systemic Lupus Erythematosus (SLE) | Methotrexate |
| Silicosis | Seronegative Spondyloarthropathies | Amiodarone |
| Coal Miner's Lung | Connective Tissue Disease (CTD) | Radiotherapy |
| Rheumatoid Arthritis (RA) | ||
*Asbestos exposure.
Usually from shipyard work or building trade.
Can result in:
- Pleural plaque: benign plaques
- Asbestosis: progressive fibrosis of lung
- Malignant lesions: e.g. mesothelioma or adenocarcinoma
Idiopathic Interstitial Pneumonitis Part 10 of 14
Idiopathic interstitial pneumonitis produces fibrosis where causative agent is unknown.
Recent theory to pathophysiology:

Histological subtypes of Idiopathic Interstitial Pneumonitis
The following are typical patterns that can be identified on histology
- Usual interstitial pneumonia: can be used by
- Idiopathic pulmonary fibrosis*
- Pneumoconiosis
- Connective tissue disease
- Nonspecific interstitial pneumonia
- Organising pneumonia (cryptogenic)
- Respiratory bronchiolitis
Idiopathic Pulmonary Fibrosis Part 11 of 14
Risk factors:
- Cigarette smoke.
- Occupational exposure e.g. coal, metal dust.
Characteristic CT findings:
- Honeycombing > 5% lung parenchyma.
- Peripheral and lower lobe predominance.
Histology:
Prognosis:
Very poor, 5 year survival between 20-40%.
Other Idiopathic Subtypes Part 12 of 14
Questions Part 13 of 14
In Summary Part 14 of 14
ILD has a restrictive pattern on spirometry.
Can be divided into known causes –
- Occupational causes leading to pneumoconiosis
- Granulomatous disease further divided into –
- Caseating – TB
- Non-caseating e.g. Vasculitis or hypersensitivity pneumonitis and sarcoidosis
, and unknown causes –
- Idiopathic pulmonary fibrosis
- Non-specific interstitial pneumonia
- Respiratory bronchiolitis
- Cryptogenic Organising Pneumonia